
- Breastfeeding
- May 27, 2026
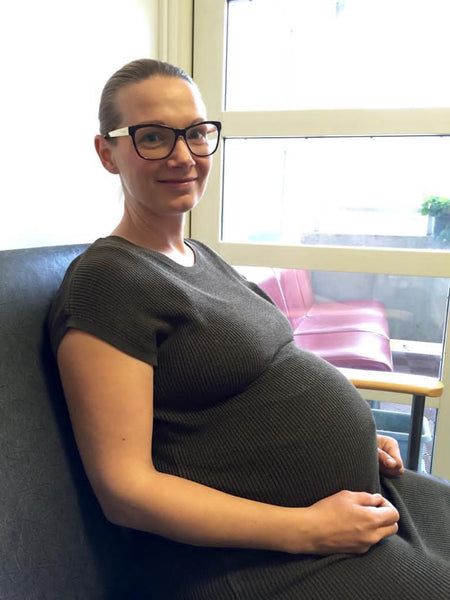
My personal story into motherhood introduces our Female Changemakers series. I recently sat down with a good friend of mine, Sanna, to discuss events that took place around the births of my children and how they affected the way I approach life these days. This written version goes into more detail about the complications I experienced, and their underlying reasons. I am hoping that this level of detail will help other mums who may experience similar issues, in particular with GBS infection.
This is not a story of a personal tragedy. I am all too conscious that many mothers go through something even worse than I did. Pregnancy and childbirth, when it goes wrong, can result in all types of horrors, including the loss of a child.
Instead, this is a story about what’s been written out of our official birth narrative. Onni’s birth, as described, would be classified in our maternity system as a success. We are made to feel that the best and only outcome from a birth is that you are both living and surviving. Yet I don´t think that´s the best outcome for mothers.
For a system that prides itself on being female-centred, our maternity care system is failing post-natal women. Not only has the physical and mental health of new mothers become secondary, but it also sometimes seems insignificant. This is a story of the suffering our maternity care system ignores.

I experienced severe complications during my first birth that were nearly fatal due to the medical team not listening to me and not giving me care I urgently needed. At 42 + 3 days overdue, I was taken into the hospital to be induced, but despite several membrane sweeps and rounds of medication, nothing happened for three full days. I remember walking up an endless number of stairs in a desperate attempt to get things going, but simultaneously grew more and more anxious about potential likelihood of complications arising from the extended period of induction. Despite several attempts, I did not feel like the medical team heard my worry.
The following morning, my waters broke and I finally thought things were moving forward. In the birth room, I was given lots of oxytocin which caused such severe contractions I was unable to move. Following this and some five epidurals, after 10 hours an infection quickly took place, sending my temperature soaring. Soon after, a wave of rigors swept over me, causing my entire body to start shaking and shivering uncontrollably. This is when my baby´s heart rate went through the roof, and the medical team decided to proceed with an urgent c-section. This was the one thing I had hoped to avoid; for the labour to take a scary turn and for complications to start to unfold at an alarming rate. I had not feared birth but instead approached it with a stern mind to bravely put up with whatever pain was to come. But when things quickly got out of my hands, I felt terrified and utterly out of control.
I have a vivid memory from the operating theatre, where due to the strong rigors, I had to be held down while being operated. I don´t think I have ever been that utterly terrified in my life. Those were the first signs of the sepsis taking hold and my body´s reaction to it. The operation felt like it went on forever, and when they finally got the baby out, there was only silence. Those seconds and minutes waiting to hear our baby cry were some of the most harrowing moments I´ve ever experienced. We waited and waited, but he didn´t cry. And from the rigors and the subsequent muscle pull in my neck from being held down during the procedure, I could not turn my head to see what was happening at the table beside us, where a growing number of doctors were attending to our son.
Our son was born semi-conscious, with a faint pulse, non-responsive and a pale bluish grey in colour. After being ventilated for about 10 minutes, he eventually started breathing on his own, and then it came; the cry. But when the nurse lifted him onto my chest – I hissed at her to take him away. I was terrified I was about to die.
What followed was a never-ending chain of threatening complications arising from the severe sepsis. Our son thankfully was given the all-clear after three days in the neonatal intensive care unit, even though there had been a strong suspicion of infection in his case. My condition however kept deteriorating: I went from developing an obstruction in my intestines to multiple organ failure within a matter of five days. The infection caused fluids to leak to my inner organs and tissues, and I became swollen like an elephant. Days at the hospital were a constant struggle between trying to rest and trying to move, as this was the only chance on my bowel regaining some movement before another operation would be needed.
When my infection rate dropped below a certain threshold, I was discharged from the maternity ward. This coincided with me feeling light-headed, like I had been drugged, with dilated pupils. The nurse shrugged off the symptoms as being something a new mum might feel after birth, as stress of the new situation. I was relieved to be going home, but at the same time wondered whether you really should feel this bad after giving birth. Even when I could not fit into my regular pregnancy clothes after birth, it didn´t register – something wasn´t as it should be. I got home an emotional mess with a blinding headache, swollen body and difficulties breathing. I started to think something was not right after all.
It was not long until I was back at the hospital: just this time at the A&E, without my baby. Turns out, this was the first time the hospital diagnosed my multiple organ failure. As a result of the sepsis and fluid leaking to my organs and tissues, the right side of my heart had doubled in size and I was having trouble breathing due to the fluid retention in my lungs. My systolic blood pressure – the cause of my blinding headache – was 220 and at that point I knew things were serious. I started to understand this was not how you are meant to feel after birth.
After days and nights at the hospital, by some miracle, my condition started to improve. With medication, my blood pressure was lowered, and the fluids finally started to exit my body. I was out of the worst, and on the way to recovery.

Afterwards, trying to make sense of what happened to me, and to address the failings in my care, I made a negligence claim to the hospital. Despite acknowledging some of the shortcomings, I never felt the hospital took responsibility for what had happened under their care – instead, I was given statistics of the many successful births they delivered every year and the supposedly marginal occasions when something went wrong. Overall, the message was that sometimes things didn´t go as planned - but that this was all part of the experience of giving birth.
There is a reasonable explanation for this apparent state of institutional denial. Birth trauma and injury conflict with the dominant maternity care ethos, that vaginal, “natural” births are safer and more empowering for women.
As the public health services keep turning a blind eye, rates of birth injury and trauma continue to rise, due to a confluence of factors including ageing mothers, obesity and larger newborns. But why isn’t more attention paid to the routine psychological and physical harm endured by so many post-natal women?
This is a question Maureen Treadwell, chair of the Birth Trauma Association, has been asking for nearly two decades. “If a man underwent dental surgery having begged for anaesthetic and not received any, we’d recommend therapy – yet if the same thing happens to a woman we tell her she’s a good girl, well done. It’s madness,” she said (the Guardian, 2017). According to Treadwell, birth trauma is exacerbated by a culture that celebrates only one kind of birth. “The system, as well as the dominant culture, fills women with false expectations. It deludes women into thinking that birth ought to be this wonderful, empowering experience and when it isn’t women feel terribly ashamed.”
Once my health improved and I got some distance to the events, I began to understand just how critically ill I had been. Once your organs start failing because of sepsis, your chance of survival drops below 50%. When later discussing my case with one of the doctors on duty that night, she bluntly confirmed that in my case, the complications had been near fatal. Had I not been in such good physical health, it would be unlikely I would be here today. I can call myself lucky for recovering from the complications at such late stage. But living or dying in such circumstances should not be down to luck.
Physically, my condition improved quickly but mentally, I still carry the scars. In those first weeks and months after the birth – despite the miraculous survival of our son - I did not feel the exhilaration that comes with a baby. I cared for my son dutifully but felt weirdly detached from everything that was happening. Looking back, I was struggling with post-traumatic stress.
It’s obvious that childbirth is deeply traumatic for many women’s minds and bodies. Just over a century ago almost 7% of pregnant women in Europe died from it. But birth is much safer now – so why are so many women still suffering its after-effects undiagnosed and untreated?
Part of the reason is that the conversation around birth trauma and injury is steeped in shame and institutional sexism. This is not just about general prudishness surrounding women’s reproductive health issues, but also a general attitude that new mothers should basically learn to suck it up.
Then there is the issue of the established practices not considering the mother or hearing her needs during birth, or afterwards. This institutional denial of women’s experience means that individual needs and complications get overlooked. It´s no wonder that when the same cookie cutter model is applied to all of us, some of us don´t fit.
Looking back at my experience, I started to see just how unprepared I had been. I had rather naively thought - a thought that was reinforced by the mainstream antenatal education - that somehow it was better not to know what might happen. How wrong had I been.
Part of the problem, I have come to believe, is that pregnant women are not properly informed of the risks of birth trauma and injury in advance.
Birth trauma is described as serious injury or damage — it can be physical or psychological (deeply upsetting and distressing) or a combination of both. Physical birth trauma can present as perineal tears, pelvic floor muscle damage, pelvic organ prolapse (POP), pelvic fractures (pubic bone, coccyx, sacrum) and caesarean wounds.
Psychological trauma can occur with or without physical trauma and can present as: postnatal depression and/or anxiety (PNDA), postpartum post-traumatic stress disorder (PTSD) and obsessive compulsive disorder (OCD); for example, having obsessive thoughts that can affect behaviour such as checking on the baby constantly or recurring thoughts that impact your enjoyment of daily life.
And while certain things can cause trauma for one woman, they may not for another depending on the care and treatment received. One of the main contributing factors to birth trauma is expectations of birth not lining up with reality. There is a lot of influence from the social media expectations of wanting a drug-free, water birth with no emergency caesarean, but it doesn't go to plan for so many of us.
I attended birthing classes before my first birth, but looking back, the information I was given was superficial at best and did not do anything to prepare me for any complications or things not going as planned. The approach was that complications only happen rarely and to the unlucky ones – so we do not want to scare you with all those gory details. There were huge gaps in the antenatal information provided, as evident in the first teary question I asked my midwife after being discharged from the hospital: Why didn't anyone tell me this could happen?
When things do not go to plan, this can easily lead to the loss of power and control. Women are in a very vulnerable position physically and emotionally at birth, and a sense of being in control can make a huge difference to the experience of birth. We need to prepare every woman with the tools, knowledge and power to have a trauma-free birth. Awareness, preparation, and access to unbiased, evidence-based information are the keys to ensuring birthing mothers can have meaningful conversations with health professionals and go on to have positive birth experiences even when things do not go as planned.
After a lengthy struggle with fertility, when we finally found out I was pregnant with our second child, we were ecstatic. However, on week 15, I developed stomach pains and a fever, and was referred to the hospital for further checks. I was seen by an Obstetrician, who after an ultrasound sent me on for further tests around the hospital. The next two days I was pushed around the hospital, spending an eternity in waiting rooms. When I finally became too weak and asked to lie down somewhere, I was begrudgingly allocated an A&E bed. In the bed, alone, I started having strong contractions and back pains – but I still did not understand just how critical the situation was. After 4 hours, and in a state of panic, I begged someone to help me. A busy doctor came in and gave me a urinary tract infection diagnosis and sent me home. Relieved to be going home, deep inside me I knew something else was happening.
Early next morning in my own bed I woke up to a feeling of fluid dripping out of me. I went to the bathroom and immediately knew my waters had broken. I did not have a urinary tract infection. I was having a miscarriage.
We rushed back to the hospital – a different one this time – where I was quickly examined. The doctor confirmed that my waters had indeed ruptured prematurely and that there was very little amniotic fluid left in my womb. The baby´s heartbeat was still there so I was allocated a hospital bed, where the reality started to slowly sink in.
For a full day I clung to hope, that by some miracle my pregnancy could go on. But when I was diagnosed with sepsis the following day, getting the baby out became urgent. I felt my world fall into pieces in a way I cannot describe. I would need to give birth to my healthy baby with a heartbeat, only for him to die in the process of me doing that.

The following days and weeks at the hospital were marked by feelings of utter desperation, incredible sense of loss and sadness. It was as if my heart had been ripped out of my chest. But something beautiful too: at this hospital, the nurses and doctors were incredibly attentive and supportive. They gave me time and consolation; they held my hand and took time to look after me. For the first time, I felt that I was being cared for as a woman, as a mother.
I also discovered that according to the normal hospital policy, a pregnant woman showing symptoms of a serious infection should always immediately be administered an IV-antibiotic – regardless of where the infection was located. I became to understand, that once again, mistakes had been made in my care.
At our request, a priest came to visit us in the hospital room with the most beautiful message. He said that had we not lost this baby, we would never meet the one who comes next. Those words gave me so much strength afterwards. The hospital placed our palm-sized baby in a little baby coffin and brought him for us to see. I got to hold him in my hand and say my goodbyes. Afterwards, our baby was cremated, and his ashes were scattered across an ´Angel Baby´ section of a nearby cemetery – this had a huge symbolic meaning to us.
The day after – the more I started to understand that maybe things did not have to end the way they did - I picked up the phone and rang the doctor I had seen first. Describing the events that had unfolded, I wanted to understand why she had chosen not to treat my symptoms. She must have been aware of the hospital policy regarding administering antibiotics in cases like mine. She explained that I had seemed physically well to her and consequently, had made a spontaneous decision not to follow the hospital policy.
This seemed insane to me as surely there was no need to fall down and scream for help every time you needed it? Except, as I started to understand, you kind of had to. For me to receive the care and attention I needed going forward, I needed to become the guardian of my own health.
After the miscarriage, in addition to the terrifying sadness and emptiness I felt, I struggled to come to terms with losing a healthy baby when things could have been different had I received the appropriate care and attention.
Medically, I felt the need to gain an understanding of my infections, so I went to see a private obstetrician who met me with immense kindness and drive to help. Under the care of this doctor, I started the process of overcoming my traumatic experiences and gaining a better understanding of my health. When referred to an infectious diseases’ specialist (the former head of the Helsinki hospital district), I learned that the underlaying cause of my infections was GBS; a very common bacteria found in both men and women that sometimes, in rare occasions, can cause serious complications like mine during and after pregnancy.
Strep B is usually only a problem if it affects pregnant women as it can harm babies before, during, and after birth. About 1 in 4 pregnant women "carry" or are "colonized" with group B strep (GBS). In very rare cases – like mine – a GBS infection during pregnancy can also cause miscarriage, early (premature) labour or stillbirth.
Babies can be infected by GBS before birth and up to about 6 months of age due to their underdeveloped immune systems. GBS most commonly causes infection in the blood (sepsis), the fluid and lining of the brain (meningitis), and lungs (pneumonia). Some GBS survivors experience handicaps such as blindness, deafness, and mental challenges, and/or cerebral palsy. Only a few babies who are exposed to GBS become infected, but GBS can cause babies to be miscarried, stillborn, or become very ill and sometimes die after birth.
A 2015 study estimated that 57,000 fetal infections/stillbirths occur annually. A separate systematic review in 2015 found that up to 12.1% of stillbirths are caused by GBS, noting that more research is needed. 12.1% of the World Health Organization's estimate of 2.6 million stillbirths per year suggests that 314,600 stillbirths may be caused by GBS, contrary to the the common thought that GBS-caused stillbirths are rare.
Although there are no official guidelines regarding prenatal-onset GBS disease prevention, several knowledge-based strategies may help prevent unborn babies from becoming infected with group B strep or other harmful microorganisms. These include:
1. Urine culturing for GBS and other bacteria
2. Knowing the signs of infection in unborn babies
3. Recognizing the warning signs and symptoms of preterm labor
4. Avoiding unnecessary invasive procedures
5. Seeing your provider promptly for an exam if you have any "vaginitis" symptoms
For more information, visit Group B Strep International.
These days, pregnant women are usually screened for GBS as part of routine prenatal care. If the results of the GBS swab test show that the bacteria is present, most women will receive antibiotics through an intravenous (IV) line once labour has started. This is done to help protect the foetus from being infected. This is however a divisive practice, with some women refusing such treatment. It is true that antibiotics carry risks and consequences for both women and babies, and this is thus a difficult decision which many women will want to weigh up and make for themselves. In my case the decision was easy: the infection left me no other choice.
I was pretty shocked to understand that back when I had my birth experiences and suffered a range of complications caused by the very bacteria – I was never screened for it. Subsequently no action was taken even though the source of the problem could have been identified with a simple vaginal swab. I am aware hospitals and even countries take different approaches to treating GBS decease – some choosing to treat cases only as problems arise, and others taking a more proactive approach. I personally feel that my experience could have been very different, had I been aware of GBS and the fact I was carrying it.
It was this approach that narrated the story of my two first births. Reacting to the worst-case scenario when it happens – because like they say, it happens so rarely. It was quite literally down to luck and this time I was the unlucky one.
But the thing is, these complications are much more common than usually recognised. Actually, poor reproductive health services are responsible for a third of all female health issues globally among women aged 15 to 44. 300,000 women die around the world because of complications of pregnancy and childbirth, every year. That is 1 woman every 2 minutes. And what more, almost all of these deaths and complications are preventable – just like mine.
Despite everything that had happened, I felt a sense of relief and strength after I started to understand what was happening to my body and why. I continued to see my private obstetrician, who, as soon as my third pregnancy started, kept a close eye on my GBS infection. From week 5 of my pregnancy the bacterial colonisation grew rapidly and so together with the infectious diseases doctor, a care plan was devised for how to ensure the continuation of my pregnancy. This included regular swab tests, treatment with antibiotics and the occasional weekend spent at the hospital in an IV-antibiotic drip. It was decided a planned c-section would be the safest way for my baby to enter the world, under the protection of antibiotics.
I spent most of my third pregnancy in a state of panic, fearing the bacteria would take hold again and history would repeat itself. But day by day, I got past important milestones, and by the time I knew the baby most likely would survive premature birth, I felt I could breathe again. But what made this pregnancy so different was that fact that I was being seen and heard, as someone with special circumstances that needed out-of-the-ordinary care.
I don´t think I have ever been as driven as I was when I was expecting Ella. I had one goal in life and that was to protect my baby and to bring her to this world safely. I was willing to do anything it took to make sure she was safe, and unharmed by the underlying infection.

When Ella was born there was no trauma, no terror, no fear, no sepsis – it was the most beautiful experience that has helped immensely to heal the trauma of the past and bring me closure. For the first time, I held my baby on my chest, soaked up the newborn scent, and felt a happiness like never before.
Finland is known for its progressive healthcare, yet a movement called #metoobirth (minamyössynnyttäjänä) has been gathering momentum here over the recent years. The movement is about women saying no to obstetric violence. Obstetric violence is described as the established practices not considering the mother or hearing her needs during birth. Then there are also the consequences of the birth, events that take place after the birth because of something that took place during delivery. This institutional denial of women’s experience is a huge problem in post-natal care, condensing the issue as “Your experience does not matter, all that matters is a healthy baby.”
Tight budgets and resources, and rigid institutional structures are visible in the birth experiences of women. There may not be time or resources to focus on the individual or meet her needs during and after birth. In fact, our system allows it that mothers are systematically ignored yet everything is being done by the book. This means that traumatic birth experiences regularly get written into the history books as successful births. Clearly there is something wrong with the system as traumatic births continue to emerge, and more and more mothers find that their experiences of birth are far from successful.
It is time we start breaking these established patterns of behaviour, where only the baby´s health is important. We need a cultural, societal shift that starts supporting mums as much as we support babies. There should be no conflict here; everyone wants a healthy baby and a healthy mum.
As recently reported by Helsingin Sanomat, the main newspaper in Finland, a Family Federation of Finland study from 2015 found that a third of mothers and a quarter of fathers of one child decided not to have more children due to a traumatic birth experience. This study supports a link between the experience of birth and declining birth rates.
The importance of the sense of being in control of your own birth experience cannot be underestimated. Satisfaction with childbirth experience is less about pain and how long labour lasted, and more about actively participating in the decision-making throughout the childbirth experience, which requires knowledge and preparation. Satisfaction with the birth experience can impact the biological process of bonding with a new baby, breastfeeding success, risk of postpartum depression, and intimacy/sexual health after baby.
By improving the experience of birth and the postpartum period, we not only improve the health and happiness of new families, but also benefit payers, providers and the society as a whole.
Historically societies have forgotten about the birth rights of the woman herself, she has become secondary. And women have somehow gotten used to this, believing that a healthy child is the only desirable outcome. The health of the baby is of course important, but a healthy baby needs a healthy mum. The two go hand in hand.
One of the biggest drivers for change, following on from the #metoo movement, is that women are finally opening up about their experiences - they are no longer silenced. It is so important that our voices are heard because those in various healthcare services are all too often muted. Thankfully, younger professionals and consumers are less willing to defer to an establishment norm, where the norm simply is not good enough. Those of us who can help, no matter how, have the drive and responsibility to do so.
They say what doesn´t kill you, makes you stronger. Well, they could not be more right. Today, I stand up stronger than ever before, determined to make a change. Understanding the shortness and unpredictability of life also makes me value every day unlike ever before. Someone wise has said that ´your second life begins when you realise you only have one´. No matter how close to dying I came, the experience has opened my eyes to a whole new reality where you need to push ahead with your dreams, aim high and seek to create a positive impact around you every day.
Since some of what happened to me was down to human error, I have found it hard to let go of the grudge I hold towards the healthcare workers I feel somehow failed me. But with time, to get closure to what happened, your focus moves to things you can influence. For me that includes learning from what happened, gaining an understanding of my own health, sharing my story with others, putting my energy into helping other mums and driving forward a change in how mothers are treated.
The main learning from my experiences has been that it all starts with awareness and preparation. By being informed you can guard and be in control of your own health; be it reproductive health or any other aspect of your health. And above all, you need to trust your instinct and learn to listen to your body.
Through this Female Changemaker series, we want to get the voices of all mums heard. We will soon be launching a campaign to encourage parents from our community to share their experiences with us.
Creating a positive, sustainable change to women´s health and to maternal care requires us to get our voices heard collectively, as mothers, as fathers and new parents. Our collective voices will be the catalyst for the positive change that starts here, today.
*Our Female Changemakers series is dedicated to individuals whose professional and personal passions have driven them to do something extraordinary, bringing sustainable positive change to women’s wellbeing. In the course of the series, I will be talking to amazing women´s health experts, professionals and parents who have gone out of their way to accelerate change and create a positive impact around them.
Please Note
The information shared in this article is intended for general educational purposes only and should not replace medical advice, diagnosis, or treatment from a qualified healthcare professional. Every pregnancy, recovery, and feeding journey is different. If you have concerns about your health, your baby’s health, or any symptoms mentioned in our blogs, please speak with your doctor, midwife, or healthcare provider before making changes to your care routine.
No additonal information available.
We offer deliveries to Europe and North America from our online store.
| Destination | Carrier | Cost | Estimated delivery | Notes |
|---|---|---|---|---|
| Finland |
Matkahuolto Postnord |
€5.90 | 2–3 business days | Home delivery: €9.90 |
| Sweden | Posti | 79 kr | 3–5 business days | Free over 999kr |
| United Kingdom | Royal Mail | £4.90 | 48 hours |
Free over £45 · Local UK warehouse |
| Ireland |
GLS DHL Express |
€9.90 €14.90 |
9–15 business days 2–3 business days |
Temporary delays with GLS |
| EU countries | GLS | €9.90 / 99 kr | 3–5 business days | Excludes Iceland, Norway, Switzerland, Cyprus, Malta, Islands of Spain & Portugal |
| Norway & Switzerland* | GLS | €9.90 | 3–4 business days | Import duties may apply |
| Cyprus & Malta | GLS | €19.90 | 2–3 business days | – |
| Iceland* | DHL Express Worldwide | from €19.90 | 2–3 business days | Import duties may apply |
| Islands of Spain | GLS | from €19.90 | 3–5 business days | Canary Islands, Baleares, Ceuta, Melilla |
| USA* | DHL Express Worldwide | $9.90 | 5–7 business days | Import duties may apply |
| Canada* | DHL Express Worldwide | $19.90 | 5–7 business days | Import duties may apply |
*Customs and import duties
Local import duties may be due at the time of delivery. These are not included in the total price paid at lolalykke.com.
Order status and tracking
You will receive an order confirmation email after purchase. A shipping confirmation email with tracking will be sent once your order has been processed and dispatched.
Change or cancel
If you need to edit or cancel your order, please contact us as soon as possible. Orders are processed quickly, so the window to make changes is short.
The rest of the world
We are unable to provide shipping outside Europe and North America at this time. Please contact us at info@lolalykke.com for further information.





